Cardiovascular disease (CVD) covers all disease processes of the heart and blood vessels. This includes heart disease, stroke and many different conditions affecting the heart and blood vessels around the body. In 2018, over 1 in 4 deaths (41,800 deaths) in Australia had a cardiovascular disease as the underlying cause. 1 CVD is the second largest contributor to the burden of disease in Australia after cancer—estimated at 14% and 18% respectively in 2015. 2
Premature CVD is highly preventable. Major modifiable risk factors for CVD include tobacco smoking, raised blood pressure, elevated blood cholesterol, insufficient physical activity, overweight and obesity, poor nutrition, drinking alcohol at harmful levels and diabetes. Socio-economic and psychosocial factors, such as low income, unemployment, remoteness, depression and social isolation are also associated with the development of CVD. In Australia, CVD is more common among disadvantaged groups. This is particularly so for Aboriginal and Torres Strait Islander people, for whom the disease burden is more than double that of non-Indigenous people. 3
A major Australian study using data up to 2015 estimated that smokers have a higher risk of most types of CVD. 4 Mortality from cardiovascular disease was almost three times higher in current versus never smokers. 4 In 2015, 11.5% of the burden of cardiovascular disease in Australia was attributable to tobacco use. 2 Over all age groups, 15% of all cardiovascular deaths in Australia can be attributed to smoking. 4 But the attributable proportion is even higher for middle-aged people. For those between the ages of 45 and 54, 38.2% of cardiovascular mortality for men and 33.7% for women is attributable to smoking. 4 Although the greatest burden is seen in middle age, smoking is a strong independent risk factor of cardiovascular events and mortality even at older age, advancing cardiovascular mortality by more than five years among smokers over 60. 5 While smoking 25 or more cigarettes per day increases a person’s risk of dying of CVD almost five-fold, even ‘light’ smoking (4–6 cigarettes per day) almost doubles a person’s risk. 4
There is now strong evidence that exposure to secondhand cigarette smoke is also a cause of coronary heart disease in non-smokers (see Chapter 4).
The key underlying pathophysiology in most cardiovascular diseases is atherosclerosis. Atherosclerosis leads to narrowing of the arteries, gradually impairing blood flow, and making the arteries harder, less elastic, and more liable to rupture. During atherosclerosis, lesions form in the walls of the large arteries that, with time, develop into plaques; build-ups of fats, cholesterol and other substances. Atherosclerosis is slow, complex and progresses with age. It often starts in early adulthood, with symptoms only arising later in life.
Cigarette smoking contributes to CVD in numerous ways, such as promoting inflammation and atherosclerosis, skewing the ratio of high and low density lipoproteins (“bad” fats versus “good” fats) in the blood, increasing blood pressure and heart rate and promoting clot formation. 6 Toxic products from cigarette smoke, in particular nicotine, carbon monoxide (CO), oxidant gases and acrolein circulate in the bloodstream. They interfere with the functioning of the endothelium (the inner cellular layer of the arterial wall), eliciting blood fat abnormalities and impairing glucose regulation. Smoking also has a direct effect on platelets (blood cells involved in the clotting process), leading to increased activation and stickiness. This in turn causes an increased risk of thrombosis, or development of blood clots. 6
Smoking a cigarette temporarily increases the heart rate and blood pressure and affects the ability of the heart to contract. These and the circulatory changes described above result in increased work for the heart muscles, which in turn raises the body’s demand for oxygen. At the same time, the body is deprived of oxygen through the effects of CO on reducing oxygen transport. The resulting imbalance in oxygen supply and demand promotes the complications of atherosclerosis. These include ischaemia (lack of oxygen due to poor blood supply), with resultant angina pectoris (chest pain or tightness) or myocardial dysfunction (poor heart muscle function). 6, 7
The 2020 report of the US Surgeon General concluded that smoking cessation reduces the burden of cardiovascular disease and the risks of cardiovascular morbidity and mortality. 8 The risk of diagnosis with any major type of CVD in Australia, for smokers who quit prior to the age of 35, was comparable to people who have never smoked. 4 In addition, smokers in Australia who quit prior to age 55 were at no greater risk of death from major types of CVD, compared to never smokers. 4 Even at older ages, quitting smoking is beneficial in reducing the cardiovascular excess risk. 5 Quitting reduces inflammation and blood clotting potential, and leads to rapid improvement in the level of high-density lipoproteins. It also reduces the development of subclinical atherosclerosis, with progression slowing as time since cessation lengthens. 8
3.1.1 Coronary heart disease
Coronary heart disease (CHD), also known as ischaemic heart disease, is the most common form of CVD. CHD was the leading cause of death in Australia in 2019, accounting for 10.8% of all deaths. 9 It occurs when the arteries supplying the heart become progressively narrowed by a atherosclerosis. This reduces the blood flow, forcing the heart to work harder to compensate, and can lead to symptoms of angina. If the plaque breaks up, a blood clot may form, blocking the artery completely. If not promptly treated, this can lead to death of vital heart muscle due to oxygen starvation (termed acute myocardial infarction or heart attack), or, in the worst case, sudden death. 6
Smoking is a cause of CHD, 10 with the most recent Australian estimates showing that current smokers are 1.7 times as likely to develop CHD, and 2.5 times as likely to experience a heart attack, compared with never smokers. 4 The risk of both increases with heavier smoking. 4 Smoking up to fourteen cigarettes per day more than doubles a person’s risk of death from CHD, while smoking more than 25 cigarettes per day increases that risk over five-fold. 4 In 2015, tobacco use was responsible for 13.9% of the disease burden due to CHD in Australia. 11 Smoking in adolescence and young adulthood is also associated with an increased risk of coronary artery atherosclerosis in adulthood. 12
Of those with CHD, smokers are more likely to die of the disease than non-smokers. A 2013 study of 50-year trends in smoking-related mortality found that although overall death rates from CHD have declined, these declines were proportionately larger for never smokers than for current smokers. The mortality rate was more than three times higher for current smokers compared with never smokers aged between 55 and 74, with two thirds of the deaths among smokers being attributable to their smoking. There was also a significantly increasing risk of CHD mortality for both men and women with increasing consumption, through 40 or more cigarettes per day. 13 The heaviest burden of excess death due to tobacco-caused CHD is felt in early middle age. In Australia, there is about a tripling in the risk of fatal heart attack in current versus never smokers aged 45–64, compared with an increased risk of 1.7 times for smokers at age 80 and over. 4 The effects of active smoking compared with no exposure are likely to be underestimated because most CVD studies have not excluded persons who had secondhand smoke exposure from the comparison group.
Lower tar and nicotine cigarettes have not been shown to reduce the incidence of CHD, due to smokers increasing the number of cigarettes smoked per day or by taking deeper, faster, more or longer puffs. Thus, such cigarettes do not provide a lower risk alternative for smokers who cannot or do not wish to quit. 6
The risks of myocardial infarction and death from CHD are lower among former smokers than among continuing smokers. The International Agency for Research on Cancer 14 describes the benefits of quitting as:
‘... there is a substantial reduction in risk of CHD compared with that of continuing smokers with the first two to four years of smoking abstinence, followed by a slower decline of risk, with risk approaching that of never smokers in fifteen to twenty years. For methodological reasons, the assessment of risk reduction is problematic within the first two years of cessation.’(p 342)
The International Agency for Research on Cancer also cites a reduced risk of 35% within two to four years for persons already suffering from CHD, and found studies on subjects without diagnosed CHD are ‘compatible with this conclusion and point toward similar relative risk reduction.’ 14 (p 336).
The 2020 Report of the US Surgeon General on smoking cessation reviewed past and more recent studies of smoking cessation on the risk of CHD. This report concluded that the risk of CHD declines rapidly in the period immediately following cessation and then declines at slower rate in the longer term. In some of the reviewed studies, the risk for CHD in former smokers eventually decreased to that of never smokers. 8
Australian research published in July 2019 found no significant elevations in the incidence of CHD in past smokers who quit by age 35, and no significant elevations in mortality from CHD in past smokers who quit by age 55. 4
There are a number of potential mechanisms by which smoking cessation may be reducing the risk of CHD. 8 Cessation stops the exposure of the cardiovascular system to the chemicals in smoke that are driving the biological processes leading to increased risk. There are immediate benefits from reduction of nicotine and CO, such as avoiding the transient increases in heart rate and CO-mediated reduction in oxygen transport. Cessation may also improve functioning of endothelial cells, 8 reducing inflammation 15 , 16 and improving the balance of lipoproteins. 17 , 18 Smoking cessation reduces the development and progression of markers of subclinical atherosclerosis, with a greater effect as time since cessation increases. 8
3.1.2 Cerebrovascular disease (stroke)
A stroke occurs when blood flow to the brain is interrupted, leading to injury or death of brain tissue. This occurs most commonly because of arterial blockage caused by atherosclerosis or a blood clot, an event known as an ischaemic stroke. Happening less often, but more likely to be fatal, is a haemorrhagic stroke, in which bleeding occurs from a leaking or ruptured arterial wall at a point weakened by atherosclerosis. Sometimes the artery stretches at the site of weakness, causing it to balloon out, forming an aneurysm. The bigger the aneurysm, the more likely it is to rupture, causing haemorrhage and a resultant stroke.
Stroke is a major cause of death and disability in Australia. One in five people experiencing their first stroke episode will die within four weeks, and one in three will die within 12 months. Among the people who survive the first month after their first-ever stroke, about half will survive five years. 19 By the end of the first year following a stroke, about half of stroke survivors still require assistance with daily activities. 19
Smoking is an important cause of stroke, with the risk of having a stroke rising with the amount of tobacco smoked. 10, 20 Smoking increases the risk of both ischaemic and haemorrhagic strokes. In Australia, current smokers are more than twice as likely to have a stroke compared with never smokers. 4 In the Australian burden of disease study, tobacco use was estimated to be responsible for 10.8% of the disease burden due to stroke in 2015. 11
As with CVD, the impact of stroke caused by tobacco is greatest among the middle-aged. In Australia in 2004–05, 41% of all deaths due to stroke in men aged between 35 and 39 were caused by smoking. The greatest impact occurred in women aged 40–44, among whom 35% of all stroke deaths were due to tobacco. 21
The 2014 report of the US Surgeon General concluded that there is causal relationship between exposure to secondhand smoke and increased risk of stroke. 22 A meta-analysis of 22 studies from this report found a relative risk of having a stroke of 1.25 for people exposed to secondhand smoke compared to unexposed people (see Chapter 4, Section 4.8.2).
In the 2020 report, the US Surgeon General concluded that smoking cessation reduces the risk of stroke morbidity and mortality. 8 The risk of having a stroke decreases steadily after quitting smoking, with an Australian study showing that those who quit prior to age 35 are at comparable risk to those who never smoked. 4
3.1.3 Peripheral artery disease
Peripheral artery disease (PAD) occurs when blockages within the blood vessels prevent proper blood circulation. PAD most commonly occurs in the legs and feet, but it can also develop in the arms and hands. It is usually caused by atherosclerosis, where fatty deposits reduce blood flow in the arteries leading to the legs. This may result in severe exertional pain (intermittent claudication), especially in the legs, reducing physical capacity and health-related quality of life. If left untreated, PAD can lead to gangrene and lower limb amputation. 23 Given that it’s the same atherosclerotic disease process, it is not uncommon for individuals with PAD to die from heart attack or stroke. 24
Smoking is an important cause of PAD, 25 with current smokers having five times the risk of developing PAD compared to people who have never smoked. 4 Smoking also reduces the success of lower limb extremity bypass grafts for PAD 26 and increases the risk of major adverse cardiovascular and limb events. 27-29 In 2015, tobacco use was responsible for 8.9% of the disease burden due to PAD in Australia. 11 There is also a strong dose–response relationship between the number of cigarettes smoked and the likelihood of developing PAD even after adjustment for other CVD risk factors. 6 Australian research using data up to the end of 2015 found that smokers of 1–14 cigarettes per day were 3.5 times as likely to experience a PAD event compared with never smokers, while those who smoked 25 or more cigarettes per day were more than seven times as likely. 4 In Australia the impact of smoking on mortality from PAD is greater in younger people. In 2004–05, about 33% of all deaths due to PAD in males aged 35-39 were attributable to smoking, as were 27% of all PAD deaths in women aged 35-39. 21
Australian research has found that smoking cessation prior to age 35 reduces a person’s risk of developing PAD to that of someone who has never smoked. 4 With cessation, the risk remains 1.5 to 2 times higher among those who quit after age 35. However, the 2020 report of the US Surgeon General concluded that the evidence is suggestive but not sufficient to infer that smoking cessation substantially reduces the risk of peripheral arterial disease among former smokers compared with persons who continue to smoke, and that this reduction appears to increase with time since cessation. 8 People who suffer vascular-related leg pain may be less likely to suffer serious obstruction of the arteries in their legs if they quit. Quitting smoking may be associated with decreased mortality and longer time before amputation for people with PAD, 30 and reduced risk of major adverse cardiovascular events in people with concurrent PAD and diabetes. 31 Quitting smoking may also reduce the risk of re-occlusion after peripheral vascular surgery. 22, 32
3.1.4 Abdominal aortic aneurysm
Abdominal aortic aneurysm is a weakening of the wall of the aorta (the major artery carrying oxygenated blood from the heart to the body) in the region below the diaphragm. The weakening occurs as a result of atherosclerotic lesions developing in the aortic wall. The wall may eventually stretch and then leak or burst. Abdominal aortic aneurysm is frequently fatal. 6
Smoking is a cause of abdominal aortic aneurysm, the risk rising with increased exposure to tobacco smoke. 10 A meta-analysis published in 2018 concluded that current smokers have almost five times the risk of abdominal aortic aneurysm, 33 while an Australian study using data up to the end of 2015 found that current smokers are six times as likely to develop abdominal aortic aneurysm, compared with never smokers. 4 Further, active smoking in adolescence and young adulthood can cause early abdominal aortic atherosclerosis in young adults. 12
Smoking cessation substantially reduces the risk of abdominal aortic aneurysm and this risk reduces with greater time since cessation. 8 Smoking is one of the few known modifiable risk factors for this disease.
3.1.5 Sudden cardiac death
Sudden cardiac death describes death occurring due to sudden, unexpected loss of heart function. Most sudden death is due to CVD, in particular CHD accompanied by smoking. Cardiac dysrhythmias (irregular muscular contractions of the heart, also referred to as cardiac arrhythmias) also cause sudden cardiac death. The US Surgeon General’s reports 6, 10, 22, 34 and a meta-analysis published in 2018 35 have reported that smokers have at least three-fold greater risk of suffering sudden cardiac death than never-smokers. Australian research has estimated that current smokers are 2.4 times as likely as never smokers to experience cardiac arrest. 4
The 2020 report of the US Surgeon General found that the evidence is suggestive but insufficient to infer that smoking cessation reduces the risk of sudden cardiac death in people without coronary heart disease. 8
3.1.6 Congestive heart failure
Congestive heart failure (CHF) occurs when the heart becomes less able to pump blood through the body effectively. The heart may become enlarged or thicken, and fluid may collect in the lungs (causing shortness of breath) or in other parts of the body (causing swelling or weight gain). CHF is usually a long-term condition that has a major impact on quality-of-life and life expectancy. CHF usually occurs in individuals with a history of heart problems such as high blood pressure or coronary heart disease. 36
As well as contributing to the disease processes that primarily lead to CHF, smoking is an independent risk factor for CHF. 10 The 2004 report of the US Surgeon General suggested that coronary heart disease (CHD) caused by smoking may contribute to heart failure. 8, 10
Australian research has found that current smokers have more than double the risk of developing heart failure compared with those who have never smoked. The risk becomes almost four-fold among smokers who smoker 25 or more cigarettes per day. 4 The effects of tobacco on deaths from heart failure are more apparent at younger ages. While less than 10% of deaths from heart failure in people 65 years and over are due to tobacco, about a third of heart failure deaths in people between 35 and 44 are due to tobacco. 21
The 2020 report of the US Surgeon General concluded that the evidence suggests but is insufficient to infer that smoking cessation reduces the risk of heart failure among former smokers compared with people who continue to smoke. There is some evidence to suggest that among patients with left-ventricular dysfunction, smoking cessation may increase survival and reduced risk of hospitalisation for heart failure. 8
3.1.7 Paroxysmal tachycardia
Paroxysmal tachycardia is a type of arrhythmia (irregular heartbeat) that begins and ends abruptly, where the heart is beating abnormally fast. It can cause an adult’s heart rate to increase from between 60 and 100 beats per minute (bpm) to between 130 and 230 bpm. Recent Australian research found, for the first time, a significant increase in the risk of paroxysmal tachycardia hospitalisation or death in current versus never smokers. Current smokers were 1.5 times as likely to develop paroxysmal tachycardia compared with never smokers. 4 It is not yet known whether smoking has a causative role in this increased risk.
3.1.8 Atrial fibrillation
Atrial fibrillation is a type of abnormal heart rhythm that starts in the upper chambers of the heart and causes them to quiver (fibrillate), instead of beating normally. This can result in the heart’s inability to efficiently pump blood. Past research on the link between smoking and atrial fibrillation has been inconsistent; however recent Australian research has found that smoking is associated with an increased risk of atrial fibrillation in a dose-dependent manner. Two recent meta-analyses, 37, 38 along with Australian research published in 2019, 4 concluded that current smokers are 1.3 times as likely to develop atrial fibrillation compared to never smokers. It is not yet known whether smoking is a cause of atrial fibrillation.
3.1.9 Other types of cardiovascular disease
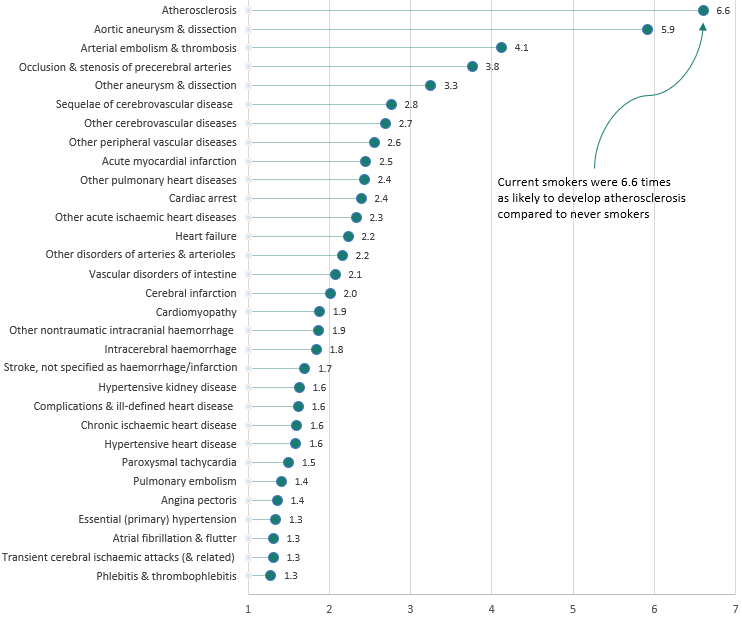
Along with the cardiovascular diseases listed above, the major Australian study published in 2019 concluded that current smoking increases the risk of virtually all CVD subtypes, at least doubling the risk of many. 4 Figure 3.1.1 shows the relative risks (i.e., how many times as likely a current smoker is to develop the CVD subtype, compared with those who have never smoked) for specific CVD subtypes, for which the risk in current smokers was statistically significant.
Figure 3.1.1 Relative risks for specific CVD subtypes in current versus never smokers
Relevant news and research
A comprehensive compilation of news items and research published on this topic
Read more on this topic
References
1. Australian Institute for Health and Welfare. Cardiovascular disease. Canberra, Australia: AIHW, 2020. Available from: https://www.aihw.gov.au/reports/heart-stroke-vascular-diseases/cardiovascular-health-compendium/data.
2. Australian Institute of Health and Welfare. Australian Burden of Disease Study: impact and causes of illness and death in Australia 2015. Australian Burden of Disease, Canberra: AIHW, 2019. Available from: https://www.aihw.gov.au/reports/burden-of-disease/burden-disease-study-illness-death-2015/contents/summary.
3. Australian Institute of Health and Welfare. Australian burden of disease study: Impact and causes of illness and death in Aboriginal and Torres Strait Islander people 2011. Australian Burden of Disease Study series no. 6. Cat. no. BOD 7, Canberra: AIHW, 2016. Available from: http://www.aihw.gov.au/publication-detail/?id=60129557110
4. Banks E, Joshy G, Korda RJ, Stavreski B, Soga K, et al. Tobacco smoking and risk of 36 cardiovascular disease subtypes: fatal and non-fatal outcomes in a large prospective Australian study. BMC Medicine, 2019; 17(1):128. Available from: https://www.ncbi.nlm.nih.gov/pubmed/31266500
5. Mons U, Muezzinler A, Gellert C, Schottker B, Abnet CC, et al. Impact of smoking and smoking cessation on cardiovascular events and mortality among older adults: meta-analysis of individual participant data from prospective cohort studies of the CHANCES consortium. Bmj, 2015; 350:h1551. Available from: https://www.ncbi.nlm.nih.gov/pubmed/25896935
6. US Department of Health and Human Services. How tobacco smoke causes disease: the biology and behavioral basis for smoking-attributable disease. A report of the US Surgeon General, Atlanta, Georgia: US Department of Health and Human Services, Centers for Disease Control and Prevention, National Center for Chronic Disease Prevention and Health Promotion, Office on Smoking and Health, 2010. Available from: https://www.ncbi.nlm.nih.gov/books/NBK53017/.
7. Benowitz NL. Drug therapy. Pharmacologic aspects of cigarette smoking and nicotine addiction. New England Journal of Medicine, 1988; 319(20):1318-30. Available from: https://www.ncbi.nlm.nih.gov/pubmed/3054551
8. US Department of Health and Human Services. Smoking cessation. A report of the Surgeon General. Atlanta, GA U.S. Department of Health and Human Services, Centers for Disease Control and Prevention, National Centre for Chronic Disease Prevention and Health Promotion, Office on Smoking and Health 2020. Available from: https://www.cdc.gov/tobacco/data_statistics/sgr/2020-smoking-cessation/.
9. Australian Bureau of Statistics. Causes of death, Australia. Canberra, Australia: Australian Bureau of Statistics, 2019. Available from: https://www.abs.gov.au/statistics/health/causes-death/causes-death-australia/latest-release.
10. US Department of Health and Human Services. The health consequences of smoking: a report of the Surgeon General. Atlanta, Georgia: US Department of Health and Human Services, Public Health Service, Centers for Disease Control and Prevention, National Center for Chronic Disease Prevention and Health Promotion, Office on Smoking and Health, 2004. Available from: http://www.cdc.gov/tobacco/data_statistics/sgr/index.htm.
11. Australian Institute of Health and Welfare. Burden of tobacco use in Australia: Australian Burden of Disease Study 2015. Canberra 2019. Available from: https://www.aihw.gov.au/getmedia/953dcb20-b369-4c6b-b20f-526bdead14cb/aihw-bod-20.pdf.aspx?inline=true.
12. US Department of Health and Human Services. Preventing tobacco use among youth and young adults: A report of the Surgeon General. Atlanta, GA: US Department of Health and Human Services, Centers for Disease Control and Prevention, National Center for Chronic Disease Prevention and Health Promotion, Office on Smoking and Health, 2012. Available from: http://www.cdc.gov/tobacco/data_statistics/sgr/2012/.
13. Thun MJ, Carter BD, Feskanich D, Freedman ND, Prentice R, et al. 50-year trends in smoking-related mortality in the United States. New England Journal of Medicine, 2013; 368(4):351-64. Available from: https://www.ncbi.nlm.nih.gov/pubmed/23343064
14. International Agency for Research on Cancer. Reversal of risk after quitting smoking. IARC handbooks of cancer prevention, tobacco control, 11 Vol. 11.Lyon, France: IARC, 2007. Available from: https://publications.iarc.fr/Book-And-Report-Series/Iarc-Handbooks-Of-Cancer-Prevention/Tobacco-Control-Reversal-Of-Risk-After-Quitting-Smoking-2007.
15. McEvoy JW, Nasir K, DeFilippis AP, Lima JA, Bluemke DA, et al. Relationship of cigarette smoking with inflammation and subclinical vascular disease: the Multi-Ethnic Study of Atherosclerosis. Arteriosclerosis, Thrombosis, and Vascular Biology, 2015; 35(4):1002-10. Available from: https://www.ncbi.nlm.nih.gov/pubmed/25745060
16. Kianoush S, Yakoob MY, Al-Rifai M, DeFilippis AP, Bittencourt MS, et al. Associations of Cigarette Smoking With Subclinical Inflammation and Atherosclerosis: ELSA-Brasil (The Brazilian Longitudinal Study of Adult Health). Journal of the American Heart Association, 2017; 6(6). Available from: https://www.ncbi.nlm.nih.gov/pubmed/28647689
17. Maeda K, Noguchi Y, and Fukui T. The effects of cessation from cigarette smoking on the lipid and lipoprotein profiles: a meta-analysis. Preventive Medicine, 2003; 37(4):283-90. Available from: https://www.ncbi.nlm.nih.gov/pubmed/14507483
18. Forey BA, Fry JS, Lee PN, Thornton AJ, and Coombs KJ. The effect of quitting smoking on HDL-cholesterol - a review based on within-subject changes. Biomark Res, 2013; 1(1):26. Available from: https://www.ncbi.nlm.nih.gov/pubmed/24252691
19. Senes S. How we manage stroke in Australia. Cardiovascular disease series no.24, cat. no. CVD 31.Canberra: AIHW, 2006. Available from: http://www.aihw.gov.au/publication-detail/?id=6442467815.
20. Doll R, Peto R, Boreham J, and Sutherland I. Mortality in relation to smoking: 50 years' observations on male British doctors. Bmj, 2004; 328(7455):1519. Available from: https://www.ncbi.nlm.nih.gov/pubmed/15213107
21. Collins D and Lapsley H. The costs of tobacco, alcohol and illicit drug abuse to Australian society in 2004/05. P3 2625. Canberra: Department of Health and Ageing, 2008. Available from: https://nadk.flinders.edu.au/files/3013/8551/1279/Collins__Lapsley_Report.pdf.
22. US Department of Health and Human Services. The Health Consequences of Smoking: 50 Years of Progress. A Report of the Surgeon General. Atlanta, GA: U.S. Department of Health and Human Services, Centers for Disease Control and Prevention, National Center for Chronic Disease Prevention and Health Promotion, Office on Smoking and Health, 2014. Available from: https://www.ncbi.nlm.nih.gov/books/NBK179276/pdf/Bookshelf_NBK179276.pdf.
23. Golledge J, Moxon JV, Rowbotham S, Pinchbeck J, Yip L, et al. Risk of major amputation in patients with intermittent claudication undergoing early revascularization. British Journal of Surgery, 2018; 105(6):699-708. Available from: https://pubmed.ncbi.nlm.nih.gov/29566427/
24. Criqui MH and Aboyans V. Epidemiology of peripheral artery disease. Circulation Research, 2015; 116(9):1509-26. Available from: https://www.ncbi.nlm.nih.gov/pubmed/25908725
25. US Department of Health and Human Services. Reducing the health consequences of smoking. 25 years of progress. A report of the US Surgeon General. Executive summary. Atlanta, GA: US Department of Health and Human Services, Public Health Service, Center for Chronic Disease Prevention and Health Promotion, Office on Smoking and Health., 1989. Available from: https://profiles.nlm.nih.gov/spotlight/nn/catalog/nlm:nlmuid-101584932X393-doc.
26. Willigendael EM, Teijink JA, Bartelink ML, Peters RJ, Büller HR, et al. Smoking and the patency of lower extremity bypass grafts: a meta-analysis. Journal of Vascular Surgery, 2005; 42(1):67-74. Available from: https://pubmed.ncbi.nlm.nih.gov/16012454/
27. Jonason T and Bergström R. Cessation of smoking in patients with intermittent claudication. Effects on the risk of peripheral vascular complications, myocardial infarction and mortality. Acta Medica Scandinavica, 1987; 221(3):253-60. Available from: https://pubmed.ncbi.nlm.nih.gov/3591463/
28. Hageman SHJ, de Borst GJ, Dorresteijn JAN, Bots ML, Westerink J, et al. Cardiovascular risk factors and the risk of major adverse limb events in patients with symptomatic cardiovascular disease. Heart, 2020; 106(21):1686-92. Available from: https://pubmed.ncbi.nlm.nih.gov/32170038/
29. Norgren L, Hiatt WR, Dormandy JA, Nehler MR, Harris KA, et al. Inter-society consensus for the management of peripheral arterial disease (TASC II). Journal of Vascular Surgery, 2007; 45 Suppl S:S5-67. Available from: https://pubmed.ncbi.nlm.nih.gov/17223489/
30. Armstrong EJ, Wu J, Singh GD, Dawson DL, Pevec WC, et al. Smoking cessation is associated with decreased mortality and improved amputation-free survival among patients with symptomatic peripheral artery disease. Journal of Vascular Surgery, 2014. Available from: http://www.ncbi.nlm.nih.gov/pubmed/25282696
31. Golledge J, Drovandi A, Rowbotham S, Velu R, Quigley F, et al. Control of modifiable risk factors and major adverse cardiovascular events in people with peripheral artery disease and diabetes. World Journal of Diabetes, 2021; 12(6):883-92. Available from: https://pubmed.ncbi.nlm.nih.gov/34168735/
32. US Department of Health and Human Services. The health benefits of smoking cessation. A report of the Surgeon General. Atlanta, GA: Centers for Disease Control, Center for Chronic Disease Prevention and Health Promotion, Office on Smoking and Health, 1990. Available from: https://stacks.cdc.gov/view/cdc/84624.
33. Aune D, Schlesinger S, Norat T, and Riboli E. Tobacco smoking and the risk of abdominal aortic aneurysm: a systematic review and meta-analysis of prospective studies. Scientific Reports, 2018; 8(1):14786. Available from: https://www.ncbi.nlm.nih.gov/pubmed/30283044
34. US Department of Health and Human Services. The health consequences of smoking: cardiovascular disease. Rockville, Maryland: Public Health Service, Office on Smoking and Health, 1983. Available from: https://profiles.nlm.nih.gov/spotlight/nn/catalog/nlm:nlmuid-101584932X318-doc.
35. Aune D, Schlesinger S, Norat T, and Riboli E. Tobacco smoking and the risk of sudden cardiac death: a systematic review and meta-analysis of prospective studies. European Journal of Epidemiology, 2018; 33(6):509-21. Available from: https://www.ncbi.nlm.nih.gov/pubmed/29417317
36. National Heart Foundation of Australia. What is heart failure? Melbourne, Australia Available from: https://www.heartfoundation.org.au/Conditions/heart-failure.
37. Aune D, Schlesinger S, Norat T, and Riboli E. Tobacco smoking and the risk of atrial fibrillation: A systematic review and meta-analysis of prospective studies. European Journal of Preventive Cardiology, 2018; 25(13):1437-51. Available from: https://www.ncbi.nlm.nih.gov/pubmed/29996680
38. Zhu W, Yuan P, Shen Y, Wan R, and Hong K. Association of smoking with the risk of incident atrial fibrillation: A meta-analysis of prospective studies. International Journal of Cardiology, 2016; 218:259-66. Available from: https://www.ncbi.nlm.nih.gov/pubmed/27236125